By Milliam Murigi
For a long time, Dr. Bernard Olayo worked in rural Kenya where providing maternal care often meant making life-or-death decisions with limited information.
Stationed in remote parts of Homa Bay County in the early 2000s, he recalls how even the most basic diagnostic tool, an ultrasound, was out of reach for most health facilities.
If a complication was suspected, expectant mothers had to travel up to 42 kilometres to access imaging services. Poor roads and limited transport used to make the journey take longer forcing many women to delay or never make the trip.
“Back then, you only saw the results much later, sometimes a week after,” Olayo recalls.
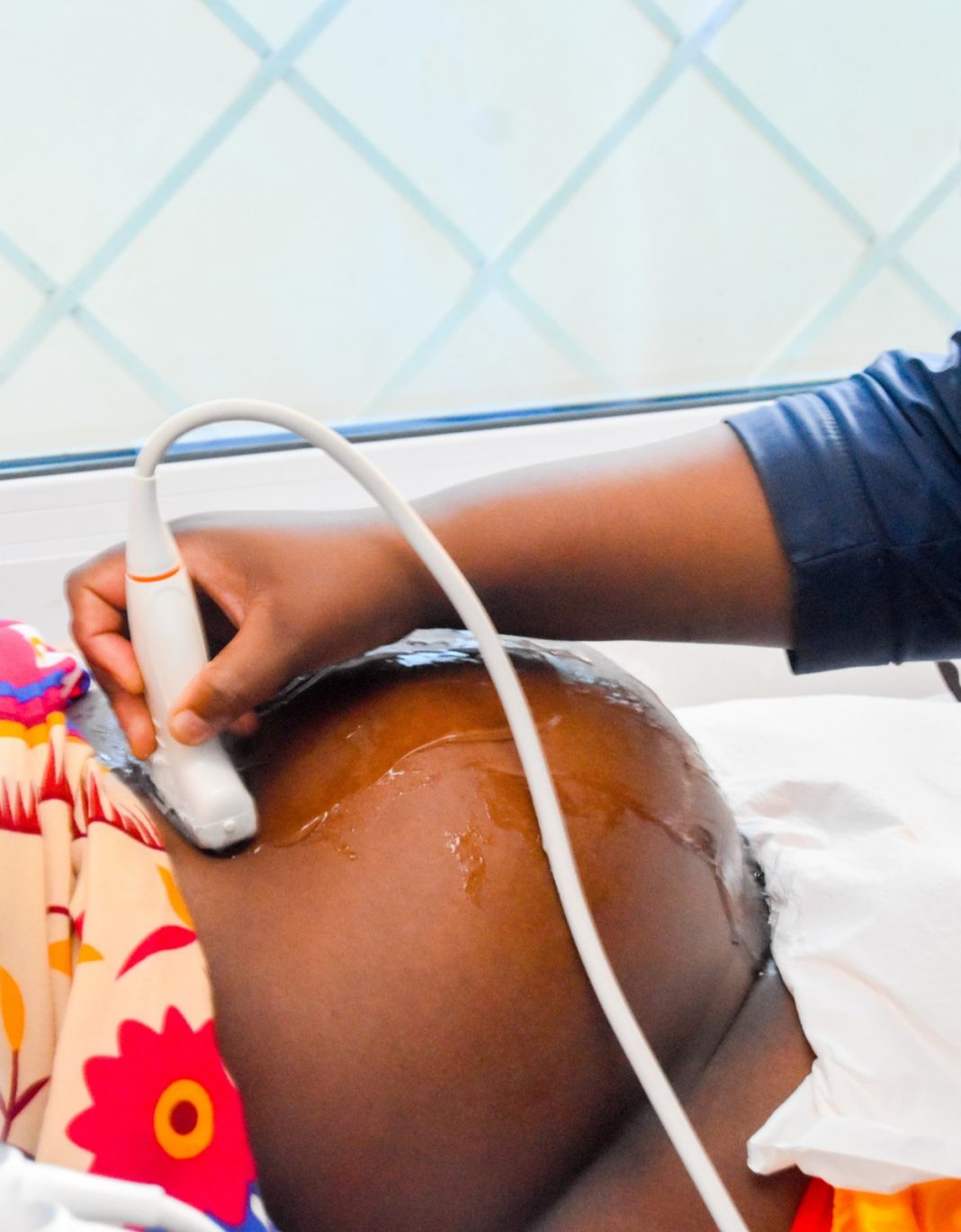
However, today, that uncertainty is being replaced by precision through Obstetric Point-of-Care Ultrasound ( O-POCUS) a portable, easy-to-use ultrasound technology designed specifically for pregnancy care by the frontline health workers.
Unlike conventional ultrasound machines that require specialized radiologists, O-POCUS devices are handheld and designed for ease of use. With built-in artificial intelligence (AI), they guide health workers through scans and generate rapid interpretations, allowing nurses and midwives to assess pregnancies in real time.
“This shift is proving critical in enabling early screening of anomalies. During routine antenatal visits, health workers can now quickly check fetal heartbeat, determine the baby’s position, identify multiple pregnancies, and locate the placenta. More importantly, they can detect warning signs early before complications become emergencies,” says Olayo.
At the core of this transformation according to him is the ability to stratify risk. With immediate access to diagnostic information, providers can distinguish between low-risk and high-risk pregnancies. This ensures that mothers who need specialized care are referred early, while others can safely continue receiving care closer to home.
But as Kenya moves from promise to practice, the conversation is shifting from pilot projects to national scale. According to Janet Karimi, who leads reproductive and maternal health at the Ministry of Health Kenya, the country can no longer afford small, fragmented pilots.
“We cannot continue doing things as usual,” she says. “We cannot keep piloting in one sub-county and calling it success. O-POCUS is currently being piloted in some counties, but the goal is to move from these pilots to full-scale implementation and generate evidence as we go.”
Karimi emphasized that the urgency is tied to global and national targets, including United Nations Sustainable Development Goals, which are now just a few years away. Accelerating progress, she notes, requires bold shifts in how innovations like O-POCUS are deployed.
She pointed out that the technology is already proving its value in detecting complications early both in mothers and newborns but cautioned that it is not a standalone solution.
“O-POCUS is not replacing routine ultrasounds,” she reveals. “It is about bringing services closer to the community and detecting complications early. But it must work within a system where once you detect a problem, you can act.”
This system includes clear referral pathways, skilled personnel and the capacity to manage complications once identified. Without these, early detection alone will not translate into better outcomes.
Karimi also highlighted the often-overlooked link between maternal health and newborn survival. A significant proportion of newborn deaths, she noted, are linked to preventable complications during pregnancy and delivery.
“If we fix the issues in the mother, we reduce newborn mortality significantly,” she says. “When a mother is pregnant, the prize is the newborn.”
This dual focus underscores why O-POCUS is being positioned not just as a diagnostic tool, but as part of a broader strategy to reduce both maternal and neonatal deaths.
Kenya has already taken key steps to enable this shift. O-POCUS has been integrated into national clinical guidelines, with recommendations for routine use during pregnancy. Training programs are underway across counties, and the technology has been incorporated into pre-service education at the Kenya Medical Training College, with plans to expand to universities.
Yet challenges remain. The cost of devices—ranging between KSh 500,000 and 1 million (US$ 3,823- 7,646)—continues to limit widespread adoption. Sustained investment, continuous training, and integration into health financing systems will be critical to ensure long-term impact.
“If Kenya is to avert the more than 5,000 maternal deaths recorded each year from conditions that can be detected and managed during pregnancy then it is high time for government to ensure that all health facilities have this device,” says Olayo.